A hospital is an institution serving patients in huge numbers daily. Serving the number of patients and maintaining their records is a must.
Patient requirements and how he’s diagnosed can be broadly divided into inpatient and outpatient. Systematic documentation of the patient belonging to any category between two becomes necessary while billing and coding.
There are people employed for this challenging task. The patient’s initial condition before admission, diagnosis, and outcome hugely vary concerning the patient’s need and depending on which it’s divided into Outpatient and Inpatient coding.
For the person seeking a career in the medical field and even, it becomes important to understand the difference and opt for a preference at first. A workplace works differently as per profession, and the job one is employed at, so the differences help to have early training and development of skills.
Key Takeaways
- Outpatient coding deals with medical procedures in a healthcare facility without requiring an overnight stay.
- Inpatient coding focuses on classifying medical services provided during a patient’s hospital or other healthcare facility stay.
- Coders for outpatient and inpatient services utilize ICD-10-CM and CPT coding systems, but outpatient coding requires additional HCPCS Level II codes.
Outpatient Coding vs. Inpatient Coding
Outpatient coding codes medical procedures and diagnoses for patients who receive treatment in an outpatient setting, such as a doctor’s clinic. Inpatient coding codes medical procedures and diagnoses for patients admitted to a hospital or other inpatient facility.

Comparison Table
| Parameters of Comparison | Outpatient Coding | Inpatient Coding |
|---|---|---|
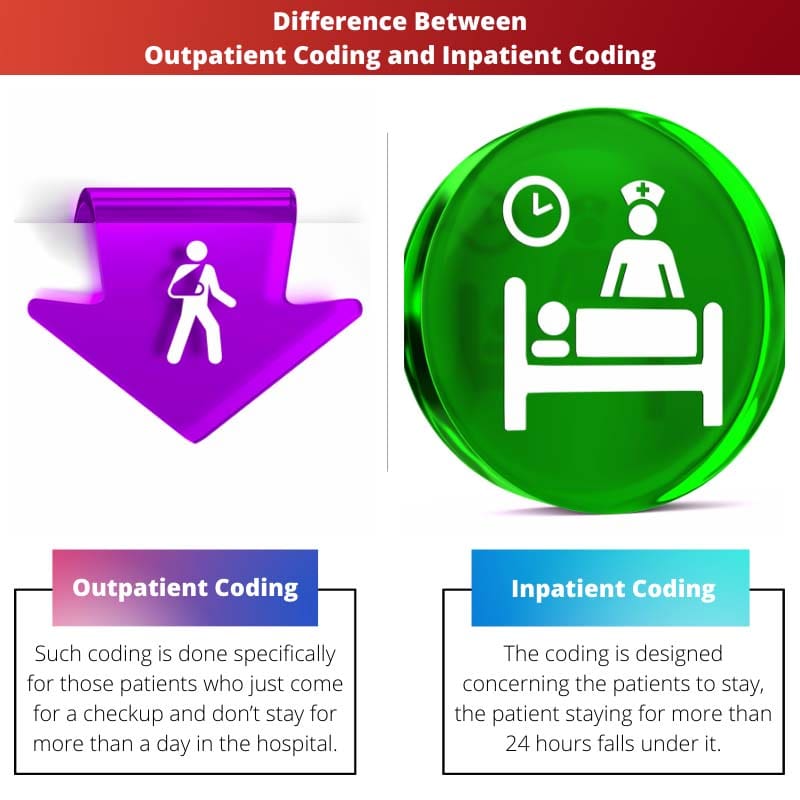
| Time of stay | Such coding is done specifically for those patients who just come for a checkup and don’t stay for more than a day in the hospital. | The coding is designed concerning the patients to stay; the patient staying for more than 24 hours falls under it. |
| Payment | Outpatient Prospective Payment System (OPPS) provides reimbursement to their respective patients. | The Inpatient Prospective Payment System (IPPS) is the method for the inpatients by their diagnosis; it’s a government and healthcare provider reimbursement plan. |
| Coding System | ICD-10-CM and HCPCS Level II codes are designed to report the details and documentation. | ICD-10-PCS and ICD-10-CM report all the essential data associated with the patient’s stay. |
| Diagnosis | The illness is not established and defined; in that case, the patient revisits for further checkups. | The diagnosis is well-defined, and the requirements and costs can be predefined. |
| Complexity | Outpatient coding is easier and less complex | Inpatient coding goes through the complexity of data arrangement and documentation for as long as the patient is hospitalized. |
What is Outpatient Coding?
Outpatient coding is a kind of medical coding used by the hospital to document the procedures performed and the requirements for the outpatients. It’s detailed reporting.
Outpatients are the people who come to seek direct treatment, taking a few hours and technically within 24 hours. The stay of outpatients in the medical facility is less, as is the complexity in the coding, but the same outpatient might frequently re-visit.
The coders seeking a job in outpatient coding require certain qualifications, and it’s necessary to have proper knowledge of coding; the most commonly used coding is ICD-10-CM and HCPCS Level II. It lacks a defined diagnosis that the coding of uncertain diseases is strictly prohibited; the coders can; however, signs and symbols can be used.

What is Inpatient Coding?
Inpatient coding is the coding system in any medical facility where the detailed analysis and diagnosis process are listed and documented precisely to ease the overall patient visit and the hospital itself. Inpatients are those admitted for a longer stay; they are hospitalized as per the diagnosis requirements.
To classify a person as an inpatient, the stay should be more than 24 hours, lasting to furthermore days. Inpatient coding requires the coder to be pro in ICD-10-PCS and ICD-10-CM coding systems.
They are the basis of the qualification criteria. The process can be complicated and complex depending upon the doctor’s prescribed stay.
All the facilities like food, medicines, and their data are registered. Inpatients can claim reimbursement under Medicare Part A; the Inpatient Prospective Payment System (IPPS) helps manage and regulate policies.

Main Differences Between Outpatient Coding and Inpatient Coding
- The main difference between Outpatient Coding and Inpatient Coding is based on the number of days and times a patient is admitted for. The outpatient coding is for the patients not staying for more than 24 hours, while the stay of inpatients is longer as the patients are formally asked to get hospitalized.
- The outpatient coding of a single patient can reoccur as the diagnosis is not well defined on the first visit, and one can be asked to visit in weeks. In contrast, the inpatient coding ends after the discharge and proper diagnosis.
- The complexity of outpatient coding is comparatively less than that in inpatient coding as inpatients start longer, and their every requirement and facility provided is well documented.
- The Outpatient coding requires the coders to know the codes and guidelines of ICD-10-CM and HCPCS Level II, whereas an inpatient coder should be pro in ICD-10-PCS and ICD-10-CM.
- OPPS (Outpatient Prospective Payment System) manages the reimbursement for outpatients for inpatients. The Inpatient Prospective Payment System (IPPS) seeks reimbursement.
- https://academic.oup.com/ajhp/article-abstract/60/suppl_6/S11/5143321
- https://onlinelibrary.wiley.com/doi/abs/10.1002/mpr.1559

Although the article is informative and well-detailed, it could be even more helpful with added examples for better understanding.
I agree, the inclusion of examples would definitely enhance comprehension.
Absolutely, examples serve as a great learning tool.
The article outlines the coding systems for outpatient and inpatient care with precision, offering valuable information for those interested in the medical field.
Absolutely, it dissects the distinct requirements of each coding system with a depth worth admiring.
The article effectively highlights the subtle differences between outpatient and inpatient coding; a beneficial resource for medical professionals.
The article’s detailed examination of the complexities involved in both outpatient and inpatient coding is highly educational.
Absolutely, the comparisons made between the two coding systems are insightful.
The comprehensive comparison between outpatient and inpatient coding provides a substantial understanding of the complexities involved in healthcare coding systems. It’s an insightful read.
It’s a well-structured explanation that delves into the intricacies of both systems, helpful for those interested in the medical field.
The in-depth analysis of outpatient and inpatient coding systems in this article certainly makes it a valuable read for individuals pursuing careers in the medical sector.
The article’s detailed exploration of the differences encompases a high level of understanding.
Definitely, its comprehensive approach to dissecting both coding systems is quite impressive.
This article brings clarity to the key differences and requirements for outpatient and inpatient coding; it’s certainly helpful for those entering the medical profession.
It’s really interesting how the article details the differences in coding in both outpatient and inpatient settings. The payment systems are explained well.
Absolutely, the article provides valuable insights into healthcare coding systems.
I found it quite enlightening, especially with the breakdown of the coding systems. The complexity of inpatient coding is well explained.
This article does a great job at explaining the difference between outpatient and inpatient coding systems and the complexities involved in both. It’s a must-read for anyone entering the medical field.
I totally agree. The way it distinguishes the requirements and differences between outpatient and inpatient systems is impeccable.
As an outsider to the medical field, I find the article’s explanation of outpatient and inpatient coding systems to be both informative and enlightening, providing a clearer understanding of the complexities within the healthcare sector.
This article serves as an enlightening reference for those venturing into the medical field, effectively dissecting the specific requirements of outpatient and inpatient coding systems.
Absolutely, its comparison of both coding systems is truly insightful.
Indeed, its breakdown of the coding complexities is commendable.
The article provides competent insights into the complexities of outpatient and inpatient coding systems, serving as a worthwhile resource for individuals in the medical sector.
I couldn’t agree more. It’s both informative and insightful.
Absolutely, it offers a comprehensive understanding of both coding practices.